In September 2017, two weeks after Hurricane Irma pummeled South Georgia, Angela Ammons discovered her hospital on life help. It was her first day as CEO of Clinch Memorial Hospital. As she walked the halls, previous outsized framed images of the close by Okefenokee Swamp, she felt relieved that the hurricane had spared the power, however overwhelmed by the rising listing of longstanding issues, from damaged tools to low employees morale. Quickly after, an auditor knowledgeable Ammons of the hospital’s ninth consecutive yr within the purple. The hospital had simply sufficient money to pay for a pair extra days of operations. With solely two of its 25 affected person beds crammed and little income coming in, Ammons didn’t know if she may make payroll. If nothing modified, she can be pressured to shut a hospital that had served the 6,650-person Clinch County, together with the small city of Homerville, Georgia, for over six many years.
“Rural hospitals are an endangered species,” says Jimmy Lewis, CEO of Hometown Well being, knowledgeable affiliation of 4 dozen rural Georgia hospitals. Clinch Memorial, he thought then, would possibly change into the state’s eighth shuttered rural hospital since 2010. Even earlier than the coronavirus pandemic halted elective surgical procedures and the revenue streams they produce, rural areas had too few insured sufferers to maintain the hospitals constructed to serve them. However their empty beds could possibly be of worth, if linked up with metropolis hospitals now going through a distinct drawback: overcapacity, particularly throughout COVID-19.
In 2017, Ammons didn’t know that simply but. She simply knew she needed to transfer quick.
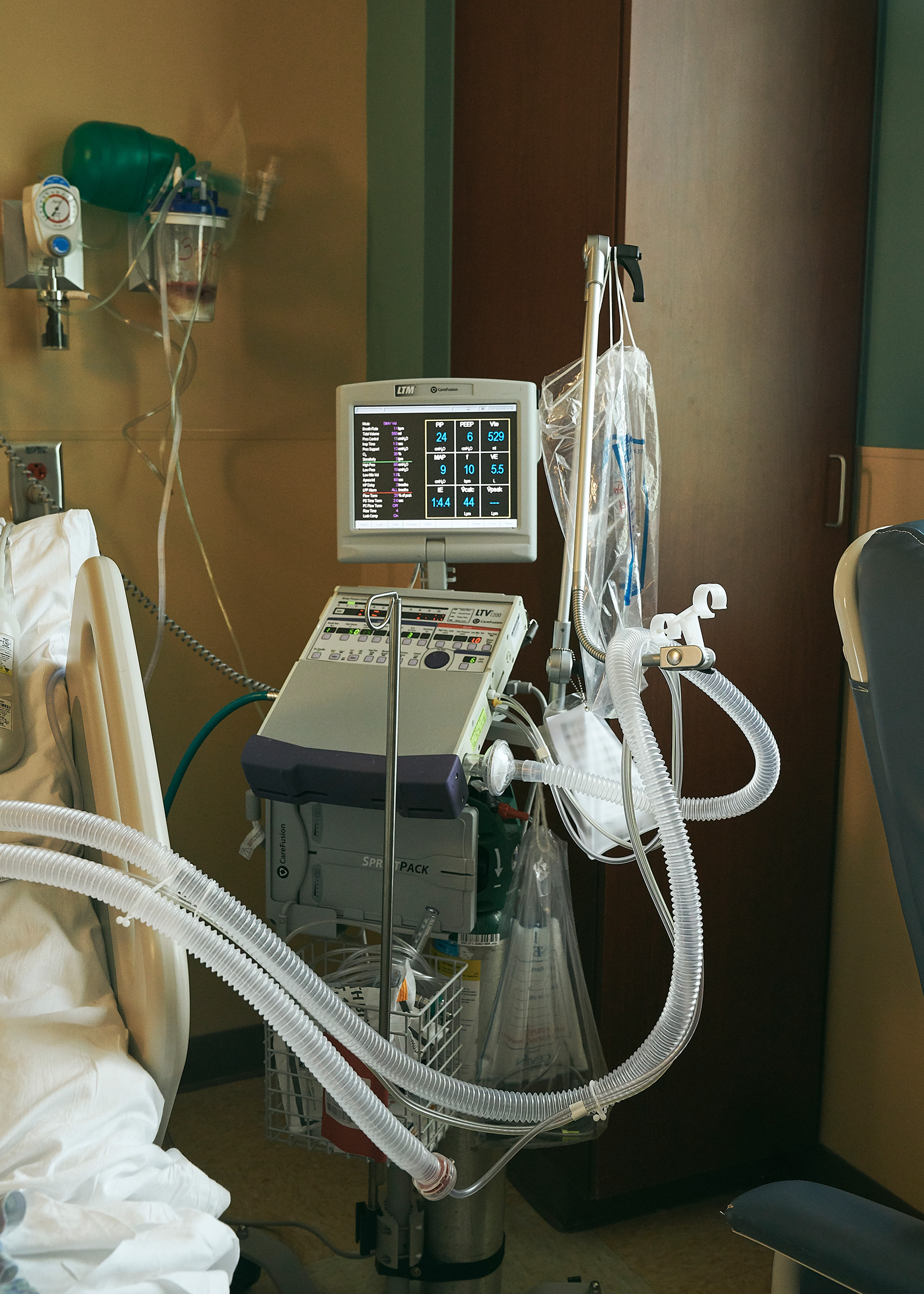
As rural hospitals had spent years on the lookout for methods to fill their empty beds, they experimented with a wide range of options to attract in sufferers from exterior their communities.
Stacy Kranitz for TIME

A member of the family visits a affected person.
Stacy Kranitz for TIME
Ammons had by no means earlier than run a hospital. The daughter of a Korean immigrant and Vietnam Conflict veteran, she was raised by her grandparents in Macon, Georgia. However their tumultuous relationship pressured Ammons to flee house at age 15. She practically turned homeless, counting on the goodwill of individuals she hardly knew to supply non permanent housing as she cobbled collectively shifts at Shoney’s. Ammons ultimately turned the primary particular person on her mom’s facet of the household to earn a school diploma. For greater than a decade, she climbed the ranks from physician’s receptionist to registered nurse supervising a staff. After the 4 earlier CEOs failed at a turnaround, Ammons satisfied Clinch Memorial’s board that her expertise overcoming hardships would offer a preventing probability at reviving the hospital.
The rookie CEO froze salaries, lower prices and picked up fee upfront for elective procedures. It wasn’t sufficient. “I used to be scared to demise, and I wanted assist,” says Ammons, conscious of the truth that closure wouldn’t solely pressure residents to journey exterior the county to the next-closest hospital, but additionally dig a knife deep into the guts of Homerville’s economic system. “We needed to do one thing totally different.”
Clinch Memorial confronted the identical issues beleaguering lots of America’s roughly 2,000 rural hospitals, which serve 57 million Individuals – a sixth of the nation’s inhabitants. The College of North Carolina’s rural well being analysis program, which has tracked over 170 rural hospital closures since 2005, discovered final yr was the worst yr for closures for the reason that Nice Recession. Practically 1 / 4 of these left are close to insolvency, in keeping with a 2019 evaluation from consulting agency Navigant. Many rural hospitals battle as a result of a majority of their sufferers are uninsured, and so they typically don’t get totally reimbursed for that care by the federal government. Obamacare gave states the choice to cowl a few of these uninsured by increasing Medicaid: Georgia didn’t. Rural hospitals are closing at larger charges in such states, whereas rural areas in states that expanded Medicaid noticed sharp declines in uninsured charges, in keeping with a 2018 Georgetown College examine.
In states that didn’t broaden Medicaid, comparable to Texas, Georgia and North Carolina, the agricultural hospital disaster pressured leaders to take excessive measures to avoid wasting services that provide not simply the one medical care in miles, however well-paying jobs. In 2014, the mayor of a small North Carolina city marched a whole bunch of miles to Washington D.C. in a long-shot bid to maintain his hospital open. In 2017, the administrator of a Tennessee hospital launched a six-figure GoFundMe marketing campaign to make payroll. Final yr, an Oklahoma hospital’s employees saved working even after the paychecks stopped coming to maintain the city afloat. Elsewhere, hospitals execs as soon as preventing over sufferers are actually collaborating with one another find methods to remain afloat. The devastating unfold of COVID-19, resulting in massive outbreaks in rural nursing properties, meatpacking crops, and prisons, have amplified the necessity for these hospitals. It has additionally exacerbated the monetary pressures lots of these services already confronted.

CPR and intubation expertise tools at Clinch Memorial Hospital.
Stacy Kranitz for TIME
As Ammons desperately searched the Web for solutions within the fall of 2017, she stumbled upon a narrative a few hospital on the opposite facet of Georgia. Two and a half hours west in Colquitt, a city even smaller than Homerville, a CEO appeared to have discovered an revolutionary strategy that exploited an inefficiency inside America’s bloated well being care system. Now these hospital beds had been stuffed with sufferers from massive southern cities, pumping new life right into a hospital as soon as in peril. Ammons didn’t totally perceive the way it labored, so she picked up the telephone and dialed the 229 space code on the Miller County Hospital web site.
A lifeline for rural communities
When MCH CEO Robin Rau picked up, Ammons wasted no time asking for assist. She sought mentorship from Rau on the right way to flip round Clinch Memorial. Rau may hear the desperation in Ammons’s voice. It resembled hers only a few years earlier.
A seasoned hospital administrator, Rau joined MCH simply because the Nice Recession began. At her first board assembly, Rau says, a lender referred to as due a word price over $3 million. Rau solely had $100,000 within the hospital’s checking account. To chop losses, Rau tried a counterintuitive resolution: supply free major care to uninsured emergency division sufferers. Although the technique required spending cash upfront, it finally lowered bills for sufferers who got here to the emergency division with minor illnesses. She then drove the greater than 200 miles to Atlanta’s Grady Memorial Hospital, which was slicing prices throughout a monetary disaster of its personal. Whereas the general public hospital was overcrowded with sufferers, Rau’s beds had been principally empty. Rau satisfied Grady to switch uninsured sufferers who had been intubated and required ongoing air flow following automobile crashes, gunshot wounds, and traumatic mind accidents – however now not wanted intensive care – to MCH.
Grady benefitted as a result of it may offload post-acute sufferers for which it obtained a decrease reimbursement price. In return, Rau may invoice the federal authorities for providing care to sufferers in MCH’s once-empty beds. She may do that as a result of MCH is a critical-access hospital – a classification that enables small hospitals situated in distant areas to be eligible for federal reimbursement as long as they deal with any affected person no matter their potential to pay. Beneath that designation, Rau may additionally “swing” her beds from solely sufferers in want of acute care to those that now not require the emergency division however nonetheless wanted extra therapy earlier than a nursing house. Although many rural hospitals employed “swing beds,” Rau was one of many first to make use of it as a serious income driver.

Services assistant James Temple within the newly upgraded laptop programs heart at Clinch Memorial Hospital.
Stacy Kranitz for TIME
The technique labored: Rau saved open her hospital’s doorways, paid off debt and expanded companies. However Rau felt cautious about divulging her technique to a different CEO. Over a decade’s time, the hospital trade had grown fiercely aggressive. City well being programs not solely expanded their affected person companies, but additionally elevated their footprints into rural areas. Rau watched as bigger programs hardly ever invested of their rural services. “I assumed, ‘Is that this going to finish up being competitors for me?’” Rau later advised TIME. However sensing Clinch Memorial had nowhere else to show, Rau agreed to assist Ammons implement a swing mattress program of her personal.
They began speaking by telephone every week, slowly turning into acquainted with one another’s hospital operations. When Rau drove to Homerville for a tour of Clinch Memorial, she was shocked and saddened by what she noticed. “There have been no sufferers, no one coming in,“ Rau says. “It was like a daggum ghost city!” By the tip of 2017, Rau’s swing mattress program that handled intubated sufferers had an extended ready listing. So she provided to ship Clinch Memorial among the sufferers who had been already being transported hours from cities like Atlanta, Jacksonville, and Tallahassee.
A type of sufferers, Derry Wells from southwest Georgia and in her early 50s, had maxed out the times insurance coverage would pay for her keep at a bigger 181-bed hospital. She may now not communicate and required a ventilator because of a worsening uncommon neurological dysfunction referred to as corticobasal degeneration. Earlier than she may go to a nursing house, her husband, Randy Wells, a minister with the Church of God, was advised about Rau’s program at MCH. Because of the ready listing, he agreed to ship Derry to Clinch Memorial, the place staffers helped her via a collection of respiratory therapies and bodily remedy.
“I’d by no means stopped in Homerville earlier than,” says Randy Wells. “There’s one thing about small-town hospitals the place they construct a greater rapport with sufferers and relations. It’s extra personable.”

Newly bought pharmaceutical hood used to combine drugs at Clinch Memorial Hospital.
Stacy Kranitz for TIME

A wishlist within the workplace of Angela Ammons, CEO of Clinch Memorial Hospital.
Stacy Kranitz for TIME
Based by a health care provider within the mid-Nineteenth century, the town of Homerville as soon as bustled because of the railroad and, later, Clinch Memorial, inbuilt 1957 with funding made out there by the Hill-Burton Act, a 1946 regulation that offered hospitals federal grants and assured loans for development. However the progress of America’s freeway system choked off life to many rural railroad cities. Homerville’s shrinking inhabitants—down 26% since 1980—slowly affected Clinch Memorial. When a brand new hospital was constructed within the mid-2000s, the board accepted a brand new facility with solely half the beds of the unique website.
From 2007 to 2009, throughout the Nice Recession, the variety of nonelderly Individuals with out insurance coverage elevated from 45 million to 50 million, in keeping with a 2010 evaluation from well being coverage journal Well being Affairs. As unemployment rose, Individuals delayed dear well being care procedures and averted hospital visits. Between 2008 and 2013, Clinch Memorial’s affected person admissions had halved regardless of the truth that Clinch County, the place Homerville is situated, is house to a few of Georgia’s worst charges of smoking, weight problems and heart problems. These outcomes, coupled with extreme physician shortages and a excessive proportion of uninsured residents, have contributed to the realm’s life expectancy of 72.7, six years youthful than the nationwide common.
Within the months following, as extra ambulances dropped off ventilator sufferers, Clinch Memorial began exhibiting indicators of life. Ammons was relieved to see her each day census develop from two sufferers to 6 – some days, it even hit double digits. However the work was simply starting. As extra out-of-town sufferers arrived in Homerville, and {dollars} flowed in from Medicare, she started to put money into the realm’s longer-term wants by planning a wellness heart, and applications that urged residents towards more healthy existence. Clinch Memorial was in a position to rent its first full-time employees doctor in over 5 years.
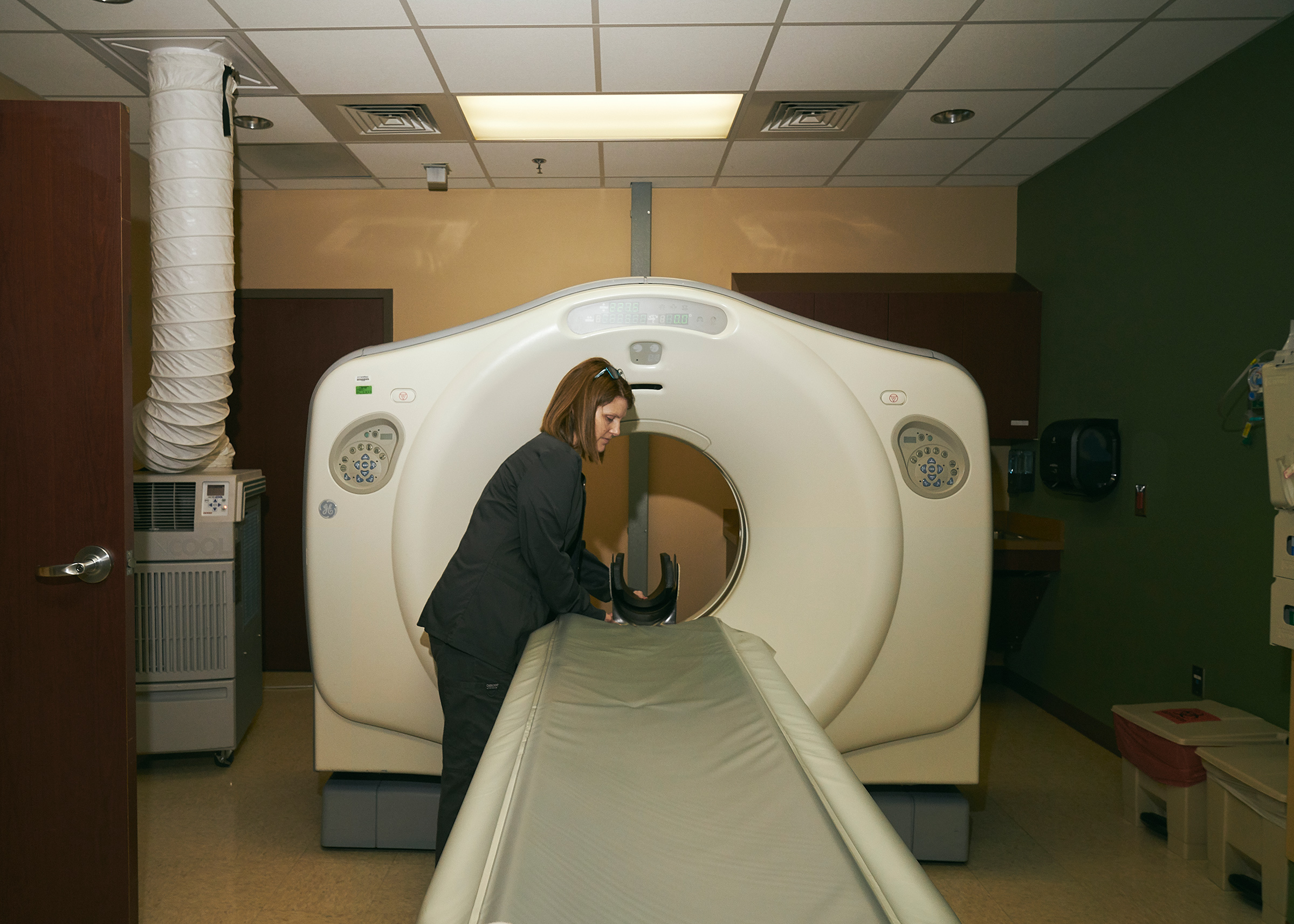
Radiology technologist Rebecca Latham with newly bought X-ray tools.
Stacy Kranitz for TIME
Hopeful as she was, Ammons wasn’t able to let her guard down. In the future final summer time, practically two years after her first day as CEO, Ammons mirrored on the hospital’s progress, however minced no phrases concerning the work nonetheless to be achieved to make sure its long-term vitality. “We’re not out of the woods,” she mentioned.
A future past higher COVID-19 care
As rural hospitals had spent years on the lookout for methods to fill their empty beds, they experimented with a wide range of options to attract in sufferers from exterior their communities. To date, few hospitals have applied the particular observe embraced by Ammons and Rau, in keeping with Mark Holmes, director of the College of North Carolina’s Cecil G. Sheps Middle for Well being Companies Analysis. However he says it suits right into a broader pattern of critical-access hospitals growing a specialty service line to “launch the pressure” from bigger services. Small rural hospitals have elevated the variety of elective surgical procedures – knee or hip replacements, for example – at a better price than different medical services. By growing that area of interest, rural hospital directors are hoping to attract sufferers away from bigger services.
“Might each critical-access hospital do [what Ammons and Rau are doing]? No.” Holmes mentioned, noting that there are solely so many extra sufferers to go round. However the broader idea “has the potential to work nationwide,” he mentioned.
This previous January, Ammons drove up for a gathering at MCH, bringing excellent news to share with Rau. Clinch Memorial was now within the black for the primary time for the reason that Nice Recession. And Ammons’s “swing mattress” program had grown practically seven-fold from revenues of $730,000 in 2017 to over $5 million in 2019. Throughout her go to, Ammons strategized with Rau, in hopes of furthering her turnaround effort. As they talked, Rau spoke freely concerning the progress she favored, providing constructive criticism wherever she noticed match. “Angela’s acquired good concepts, totally different concepts, some that I wouldn’t do exactly but,” Rau mentioned, referring to Ammons’s choice to supply holistic companies comparable to spa or therapeutic massage remedy. “I fear about her spreading herself too skinny.”
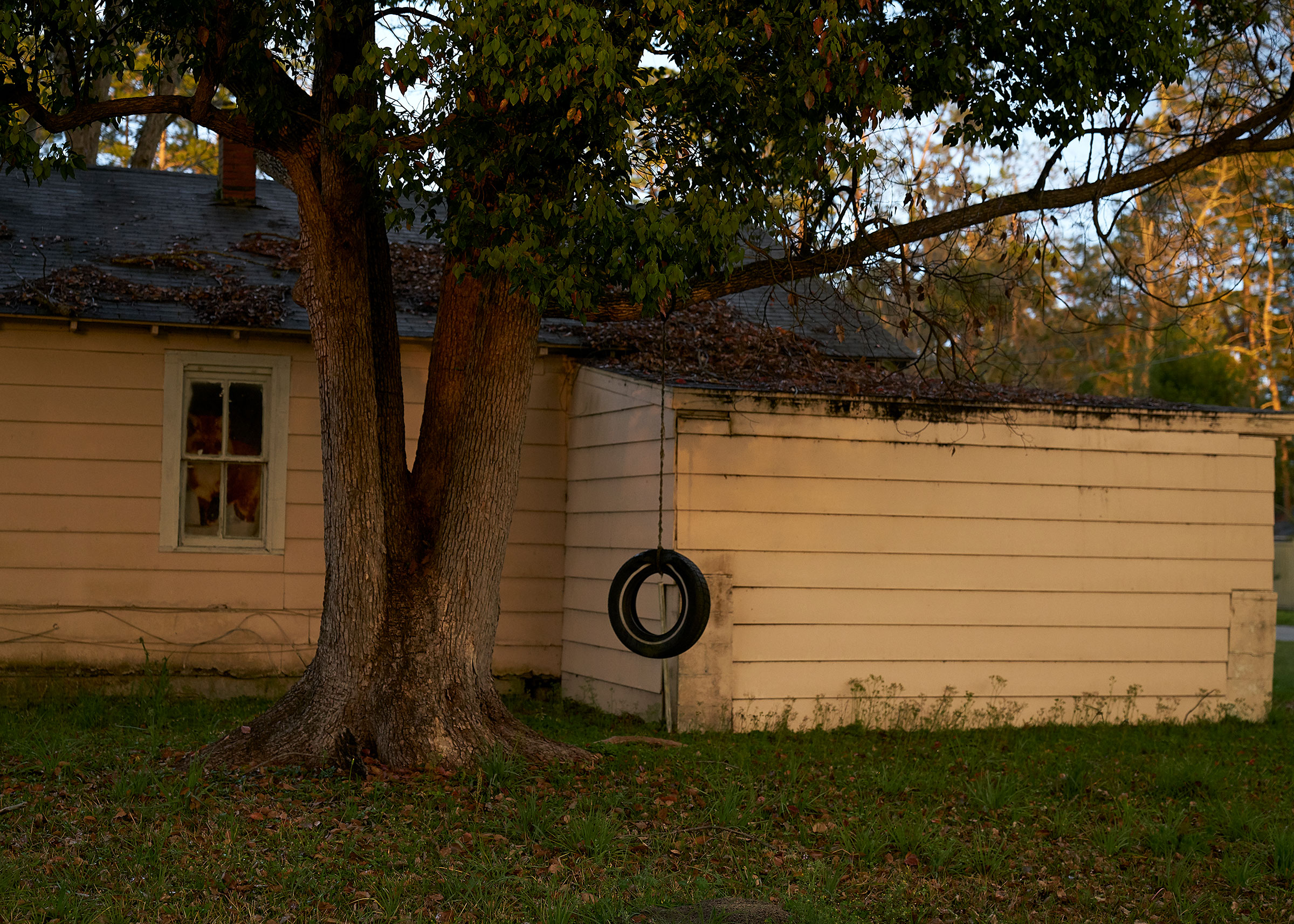
The inhabitants of rural Homerville, Ga. is now down 27% since 1980, which has damage its hospital, Clinch Memorial.
Stacy Kranitz for TIME
By the point COVID-19 arrived in Georgia, Ammons was prepared to reply. Clinch Memorial may now settle for bigger hospitals’ sufferers who had been already on ventilators however didn’t have the infectious illness. Originally of the pandemic, the swing mattress program drew in over $1 million in month-to-month revenues, which offset losses attributable to the state’s non permanent ban on elective procedures throughout its shutdown.
This previous summer time Georgia’s COVID-19 instances surged to document ranges, a lot in order that hospitals had been solely full. So when Ammons realized a hospital in close by Waycross had diverted sufferers, she provided to take a few of their non-COVID-19 sufferers to unencumber house. They agreed. For the primary time since Ammons arrived in Homerville, Clinch Memorial’s beds had been now full, and sufferers who would possibly’ve been left ready for a mattress at different hospitals acquired admitted sooner.
“I do know that many are simply attempting to outlive the each day, however we are able to’t overlook that we’ll get previous this,” Ammons mentioned. “This pandemic has impressed a number of innovation that we’ll use for years to come back.”















